Powered by People Who Care
Closer connections for people with Medicare and their health plans.

Bloom delivers High Value Enrollment
We are reshaping how government-sponsored health plans and their stakeholders approach enrollment and pre-effective engagement to sustain growth and improve retention.
Our SolutionsLet’s make things better every step of the way.
Telesales
Grow your health plan sales and give shoppers an enrollment experience tailored to their needs, with the right conversation.
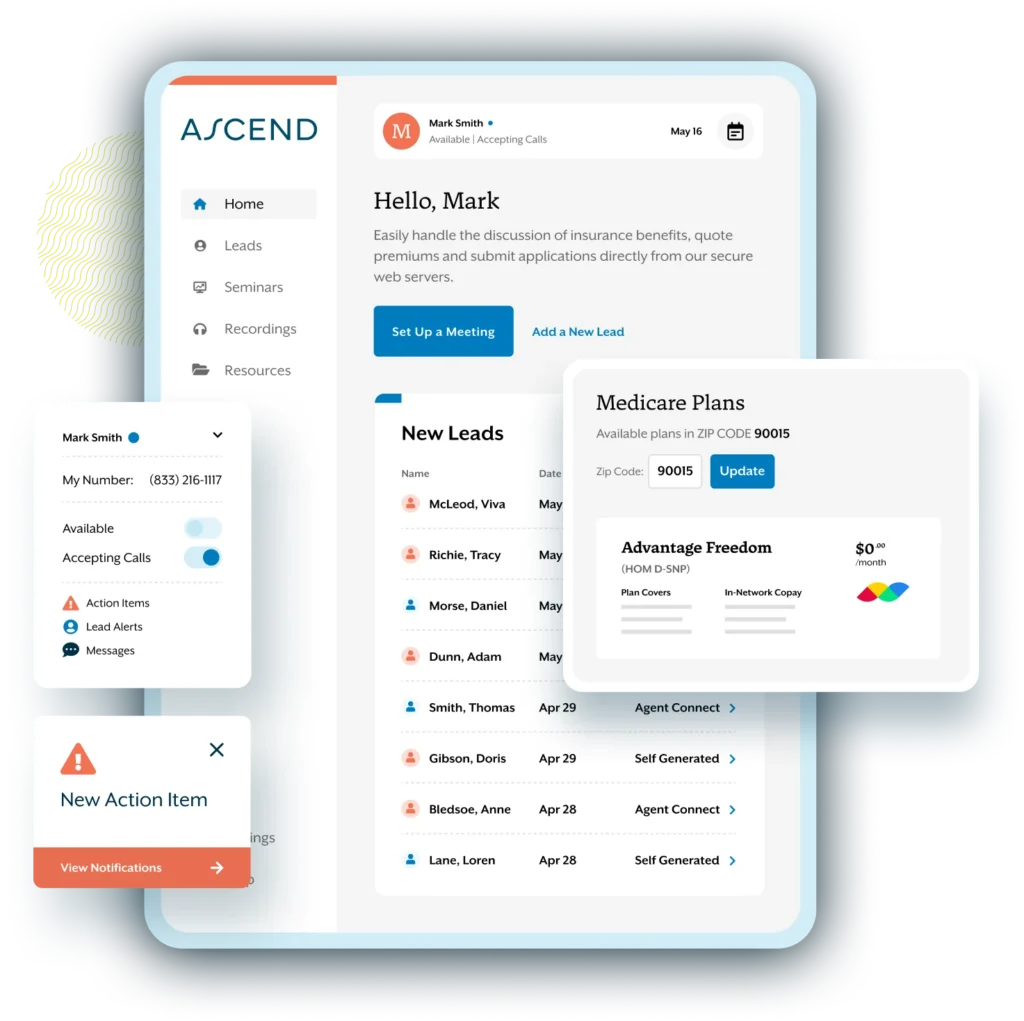
Ascend Quote & Enroll
Use our industry-leading technology to provide seamless quoting, enrollment, and early engagement.
Health Activations
Connect with members anywhere along their journey to conduct meaningful interactions, gain actionable health insights, and boost care readiness.
Purpose-built platform to accelerate growth.
Let’s combine technology with human insights for a better shopping, enrollment, and engagement experience.
Health plans grow when people thrive
- Reduce Enrollment Fallout
- Understand What People Really Need
- Help Members Access Care Earlier
- Improve STAR Ratings, Boost Revenue
Careers
Work virtually. Help real people.
Jumpstart a flexible and fulfilling career with growth opportunities and a people-first culture.

Want High Value Enrollment? Let’s start at the beginning.
Find out how pre-effective engagement drives healthier outcomes for all.